How is epilepsy managed?
Medications
Many children with epilepsy effectively manage their seizures with medications. As many as 3 out of every 4 children with epilepsy may be able to remain seizure-free with medication alone. Dozens of medications are used in the treatment of epilepsy, and those drugs have been used in a wide variety of different combinations. The kind of medication that is prescribed is determined by the kinds of seizures taking place and other physical symptoms. Unless a patient's seizures are especially severe, it is typical for the lowest known effective dose of a single medication to be prescribed. Every drug has side effects and risks, so it is safest to start treatment with the smallest dose possible. If initial treatment is not effective, your doctor will either increase the dose, switch medications, or add an additional drug. It is not unusual for patients to have their medications adjusted several times as they begin treatment for epilepsy.
It is important to discuss several details regarding your anti-epilepsy medication regimen with your doctor including what to do if you miss a dose, potential side effects, warning signs and symptoms, and known drug interactions. Medication regimens for epilepsy can be complex, and it is important to know these details to be safe. Your health care team will provide you with all the details you need.
In addition to scheduled medicines that help prevent seizures, your doctor will also prescribe a rescue medication to stop any seizures that last 5 minutes or longer. Rescue medications should be available at home and at school, and should be available to the child whenever possible.
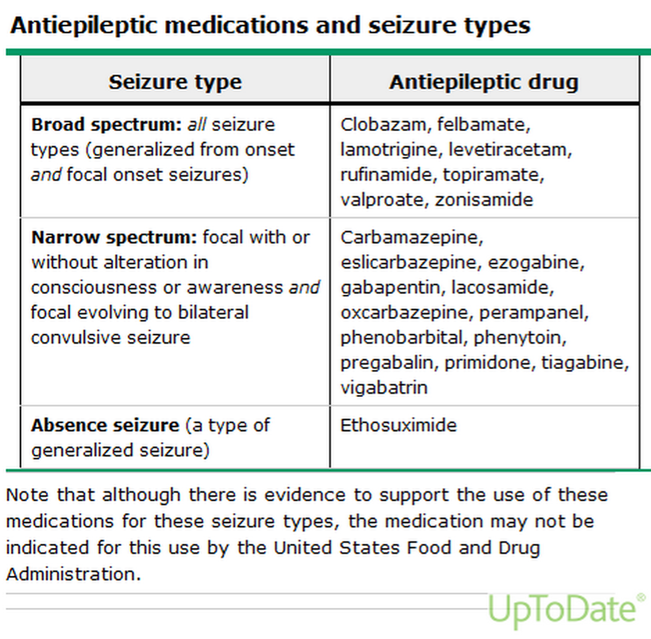
For reference, a chart matching seizure types and common anti-epilepsy medications is provided below. Medication changes should not be attempted without the consultation of a qualified health care professional.
Many children with epilepsy effectively manage their seizures with medications. As many as 3 out of every 4 children with epilepsy may be able to remain seizure-free with medication alone. Dozens of medications are used in the treatment of epilepsy, and those drugs have been used in a wide variety of different combinations. The kind of medication that is prescribed is determined by the kinds of seizures taking place and other physical symptoms. Unless a patient's seizures are especially severe, it is typical for the lowest known effective dose of a single medication to be prescribed. Every drug has side effects and risks, so it is safest to start treatment with the smallest dose possible. If initial treatment is not effective, your doctor will either increase the dose, switch medications, or add an additional drug. It is not unusual for patients to have their medications adjusted several times as they begin treatment for epilepsy.
It is important to discuss several details regarding your anti-epilepsy medication regimen with your doctor including what to do if you miss a dose, potential side effects, warning signs and symptoms, and known drug interactions. Medication regimens for epilepsy can be complex, and it is important to know these details to be safe. Your health care team will provide you with all the details you need.
In addition to scheduled medicines that help prevent seizures, your doctor will also prescribe a rescue medication to stop any seizures that last 5 minutes or longer. Rescue medications should be available at home and at school, and should be available to the child whenever possible.
For reference, a chart matching seizure types and common anti-epilepsy medications is provided below. Medication changes should not be attempted without the consultation of a qualified health care professional.
Diet Therapy
For children whose seizures are not well-controlled by medication, dietary treatment is often the next option. Several low carbohydrate diets are used to treat epilepsy including the Modified Atkins Diet, Low Glycemic Index Diet, and Ketogenic Diet. Of these diet options, the Ketogenic Diet is the most studied and most used in treatment facilities.
The Ketogenic Diet is a low-carbohydrate, high-fat diet that is very dissimilar from normal diets, and is especially different from typically low-fat Asian cuisine. Preparing food requires precise measurement using a digital scale to ensure that the patient is receiving the right amount of fat, protein, and carbohydrates. In addition, patients on the Ketogenic Diet are required to perform regular blood glucose and urine ketone tests. If your child is prescribed the Ketogenic Diet, he or she will be assigned a team including a neurologist, pharmacist, and dietitian to help provide all the necessary training to be successful.
For those seeking more technical information, an articled entitled The Ketogenic and Atkins Diets: Recipes for Seizure Control provides a history of the diets and describes their use.
Surgery
If two or thee anti-epileptic medications have failed to control your child's seizures, he or she may be a good candidate for surgery. The goal of surgery is usually to remove the area of the brain that is experiencing abnormal electrical activity. However, if your child has seizures that affect the whole brain, other useful operations are available. Surgery is only used in patients whose seizures are not controlled by medication. A full examination by the neurosurgery team is necessary to determine if your child is a good candidate for surgery.
Vagus Nerve Stimulator (VNS)
A vagus nerve stimulator is an implanted device that sends an electrical signal to activate the vagus nerve when it detects a seizure coming. The vagus nerve then sends an impulse to the brain stem, which can stop the seizure from occurring. Vagus nerve stimulators are typically only used in patients with partial seizures, who are over 12 years old, and whose seizures are not controlled by medication. In most cases, the vagus nerve stimulator is implanted in the left chest wall, and a wire is threaded under the skin in the neck where an electrode connects to the left vagus nerve.
For children whose seizures are not well-controlled by medication, dietary treatment is often the next option. Several low carbohydrate diets are used to treat epilepsy including the Modified Atkins Diet, Low Glycemic Index Diet, and Ketogenic Diet. Of these diet options, the Ketogenic Diet is the most studied and most used in treatment facilities.
The Ketogenic Diet is a low-carbohydrate, high-fat diet that is very dissimilar from normal diets, and is especially different from typically low-fat Asian cuisine. Preparing food requires precise measurement using a digital scale to ensure that the patient is receiving the right amount of fat, protein, and carbohydrates. In addition, patients on the Ketogenic Diet are required to perform regular blood glucose and urine ketone tests. If your child is prescribed the Ketogenic Diet, he or she will be assigned a team including a neurologist, pharmacist, and dietitian to help provide all the necessary training to be successful.
For those seeking more technical information, an articled entitled The Ketogenic and Atkins Diets: Recipes for Seizure Control provides a history of the diets and describes their use.
Surgery
If two or thee anti-epileptic medications have failed to control your child's seizures, he or she may be a good candidate for surgery. The goal of surgery is usually to remove the area of the brain that is experiencing abnormal electrical activity. However, if your child has seizures that affect the whole brain, other useful operations are available. Surgery is only used in patients whose seizures are not controlled by medication. A full examination by the neurosurgery team is necessary to determine if your child is a good candidate for surgery.
Vagus Nerve Stimulator (VNS)
A vagus nerve stimulator is an implanted device that sends an electrical signal to activate the vagus nerve when it detects a seizure coming. The vagus nerve then sends an impulse to the brain stem, which can stop the seizure from occurring. Vagus nerve stimulators are typically only used in patients with partial seizures, who are over 12 years old, and whose seizures are not controlled by medication. In most cases, the vagus nerve stimulator is implanted in the left chest wall, and a wire is threaded under the skin in the neck where an electrode connects to the left vagus nerve.
Other Care
Managing epilepsy requires attentive care. For some medications to be effective, they need to be taken on a strict schedule. Some medications are much less effective if they are not taken within 30 minutes of their scheduled time.
In addition to medication management, patients with epilepsy need to be aware of what triggers their seizure episodes. With planning, it is possible to avoid most triggers. Common triggers include missed medication doses, lack of sleep, stress, and alcohol use. For teenagers with epilepsy, it is especially important to stress that alcohol use can trigger a seizure. All people with epilepsy need to be mindful of their bodies by getting adequate rest, hydration, and nutrition. Managing stress also requires maintaining an active social support network.
Finally, it is recommended that people with epilepsy wear a medical bracelet to alert emergency medical services about their condition and provide them with information about what medications to administer in case of an emergency.
Managing epilepsy requires attentive care. For some medications to be effective, they need to be taken on a strict schedule. Some medications are much less effective if they are not taken within 30 minutes of their scheduled time.
In addition to medication management, patients with epilepsy need to be aware of what triggers their seizure episodes. With planning, it is possible to avoid most triggers. Common triggers include missed medication doses, lack of sleep, stress, and alcohol use. For teenagers with epilepsy, it is especially important to stress that alcohol use can trigger a seizure. All people with epilepsy need to be mindful of their bodies by getting adequate rest, hydration, and nutrition. Managing stress also requires maintaining an active social support network.
Finally, it is recommended that people with epilepsy wear a medical bracelet to alert emergency medical services about their condition and provide them with information about what medications to administer in case of an emergency.